Chapter 2: Doctors Who Diagnose and Treat Obstructive Sleep Apnea.
Introduction
In this chapter we will try to answer a few questions you may have about:
- which doctors first see patients,
- prescribe tests,
- diagnose sleep apnea,
- decide treatments etc..
So, without preamble, here we go…
Who first sees a sleep apnea patient?
The closest doctor to you and your family initiates the process that may ultimately lead to a treatment,
… yes, you understood correctly…. your primary care doctor is usually the first one to suspect the presence of the disease.
Why?
First, it is very likely that he has known you, and hence your medical history, for a long time.
Second, sleep disorders affect an ever-increasing number of people. He has thus probably honed his skills.
He is usually knowledgeable about the symptoms, consequences, risk factors etc.
It is this doctor who will first gauge whether you may be suffering from sleep apnea. He will then decide whether you may need more exams and possibly treatment.
So, based on an analysis of your symptoms, he/she will then decide whether to refer you to a sleep specialist for a thorough examination.
But your dentist may also play a significant role… let’s see how.
Can a dentist diagnose sleep apnea? What is his role in OSA treatment?
A dentist cannot make a full diagnosis of OSA. Though, he can still identify whether you could benefit from treatment.
And that is because he can examine oral and anatomical structures playing a role in sleep apnea.
Also, he sees more than 50% of the population twice a year.
He can thus help identify many patients at risk.
So, what will he do if he thinks you suffer from OSA?
Simple!
Just as for your primary care doctor, a dentist will refer you to a sleep specialist, for a thorough examination. This will allow him to decide whether if you really suffer from sleep apnea.
But the role of dentists does not end there.
Your sleep specialist may send you back to your dentist.
That is, provided your dental specialist is certified by the American Board of Dental Sleep Medicine (ABDSM) (see below).
Typically, you will see a certified dentist after the failure of CPAP (see Chapter 4: Treating obstructive sleep apnea (OSA) with CPAP and dental appliances.).
CPAP is the first line of treatment for obstructive sleep apnea
But before stopping CPAP, you need to talk to your sleep doctor and/or supplier of a CPAP machine.
Why?
Because it often happens that minor fine-tuning of the machine or adjustments of the mask will be enough to make you want to stick to CPAP.
If CPAP is really not for you, then you should contact a dentist who makes dental appliances.
These are devices that keep your airways open during sleep and ease airflow.
After that, you are done, and no longer need to see anyone, right?
Well, not quite.
After starting to wear a dental appliance, consider follow-up visits with your dentist.
This will ensure that the device is well fitted and that it does not lead to:
- teeth displacement from their normal alignment,
- bleeding gums;
- other gum diseases.
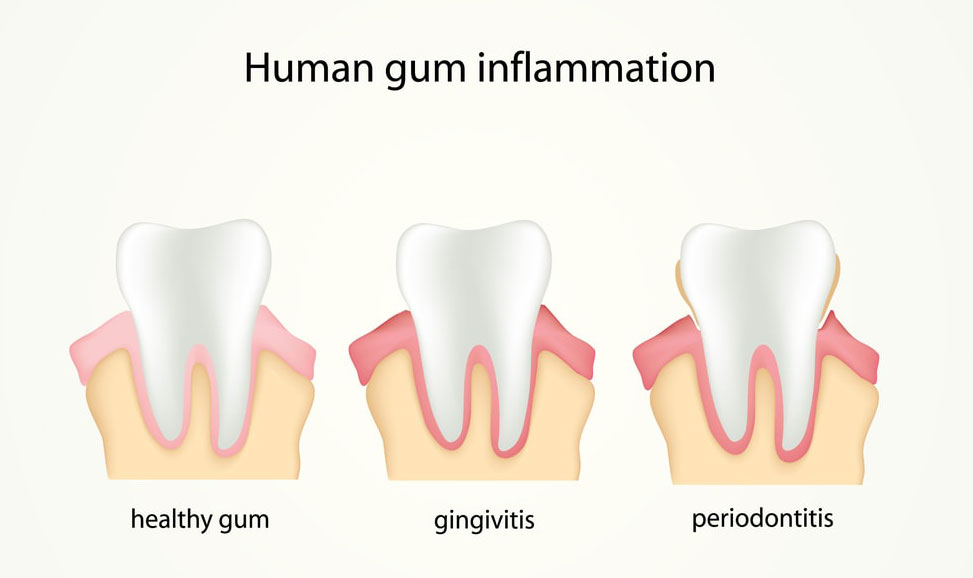
We mentioned board certification for dentists. So that brings us nicely on to the next section.
Which dentists can treat snoring and sleep apnea?
Only a few actually.
I’ll hazard a guess, you are wondering why right?
Because sleep medicine is a young multidisciplinary science.
And also because, as we said above, your dentist needs to undergo specific training.
This is important since he will have to collaborate with other specialists.
Also, he must understand oral appliance therapy very well.
Interestingly, this training does not belong to the nine dental specialties recognized by the American Dental Association.
Instead, a dental specialist will receive certification:
- by the American Board of Dental Sleep Medicine (ABDSM),
- or by the Academy of Dental Sleep Medicine (USA).
The American Academy of Sleep Medicine (AASM) recognizes these degrees.
But only a few dentists have treated enough patients to be able to claim the necessary level of experience.
So, you may have to investigate a little further before deciding.
We mentioned the role of a sleep specialist several times already. So, you are probably curious to know more, by now.
Let’s thus look at this medical profile and see what he does.
Who is a sleep specialist and what role does he play?
Before we answer that, here is another quick question for you: how many sleep disorders do you think there are?
Anywhere between 70-100 according to different sources! (100 according to the Stanford Medical Center).
These include the following more common disorders:
- sleep-disordered breathing, including obstructive sleep apnea,
- snoring,
- restless legs syndrome,
- chronic insomnia,
- narcolepsy/cataplexy and other forms of hypersomnia
and many more …

types of sleep disorders
And the numbers of people affected are equally impressive….…
………. 25-30% of all Americans across all demographic groups (children, teenagers, adults, elderlies).
That is a whopping 50-70 million Americans chronically suffering from a sleep or a circadian disorder.
And most of them go undiagnosed despite its proven negative effects on people’s health such as:
- disabilities,
- related diseases,
- and even mortality.
No wonder that doctors are trained specifically to diagnose and treat people who have sleep problems.
These doctors are called… suspense … sleep specialists. What a surprise! ?
Interestingly, Sleep Medicine has only recently been recognized as a specialty of medicine.
Board certification of practitioners dates to 1978.
This is because the physiology of sleep was fully understood only a few decades ago.1
For instance, REM sleep was discovered in the 1950s and circadian rhythm disorders in the 70s.
Hence standards were introduced in the seventies.
Sleep medicine is now a sub-specialty within several medical disciplines such as:
- internal medicine,
- anesthesiology,
- psychiatry and neurology,
- pediatrics,
- family medicine,
- otolaryngology.
So, to become a sleep specialist, you need further training in sleep medicine, and you will learn to:
- diagnose,
- treat,
- manage,
- help prevent,
the numerous sleep disorders we referred to above.
One of the reasons you need to become competent is the challenge due to the presence of many disorders with similar symptoms.
For instance, excessive daytime fatigue and sleepiness are always an observed symptom. This is true unless sleep deprivation is deliberate.
So, if you are a sleep specialist, you will be able to make a correct diagnosis of sleep disorders to identify the best treatments.
As explained above, a correct diagnosis will depend on:
- a physical exam,
- medical history,
- and then some further tests or sleep studies such as a polysomnogram.
Technicians will perform some of these tests and sleep studies. Sleep specialists will then interpret the data.
Treatments may include:
- oral appliances,
- changes in your lifestyle such as losing weight,
- continuous positive airway pressure (CPAP)…
You will find your sleep specialist working in sleep clinics, also called sleep laboratories or centers.
These can be privately-owned or affiliated with existing hospitals or medical centers.
Final remarks
We hope you have enjoyed this article.
By now you should have a good idea of which doctors are involved in the diagnosis and treatment of OSA.
Let us know whether you have any questions.
Consider heading over to the natural continuations of this chapter, namely:
- Chapter 3: Diagnosis of Obstructive Sleep Apnea (OSA).
- Chapter 4: Treating obstructive sleep apnea (OSA) with CPAP and dental appliances.
- Chapter 5: Treating Obstructive Sleep Apnea (OSA) with Surgery.
Though consider taking a peek at the following more introductory articles, if you have not already done so:
Chapter 1: Obstructive Sleep Apnea (OSA) and its Health Effects.
Obstructive Sleep Apnea: The Definitive Guide for 2020.
SUTTON PLACE DENTAL ASSOCIATES ON THE WEB